Thursday May 8, 2014
Today is World Ovarian Cancer Day, and on this day, ovarian cancer organisations from around the world unite to educate their communities about ovarian cancer and its symptoms
BY DR SURESH KUMARASAMY
 |
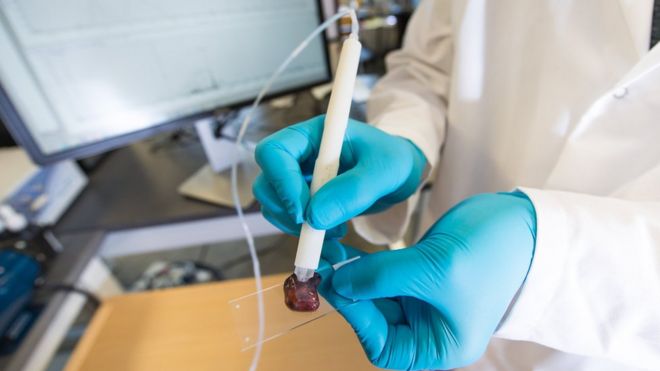
Working at it: There is ongoing research evaluating a combination of blood tests for tumour markers together
with ultrasound scans with the hope of developing a screening test for ovarian cancer in the future. — AFP |
Each year, nearly a quarter of a million women around the world are diagnosed with ovarian cancer, and the disease is responsible for 140,000 deaths annually.
Statistics show that just 45% of women with ovarian cancer are likely to survive for five years, compared with 89% of women with breast cancer.
Recognising the severity of the disease and the need to raise awareness about ovarian cancer, the first World Ovarian Cancer Day was organised on May 8, 2013.
On this day, ovarian cancer organisations from around the world unite to educate their communities about ovarian cancer and its symptoms.
Today marks the second annual World Ovarian Cancer Day, and for women living with the disease, and their families and friends, this day has built, and will continue to build, a sense of solidarity in the fight against the disease.
The theme for 2014 is “One Voice for Every Woman”.
Ovarian cancer is a cancer of the female reproductive system, and is the fifth most common cancer among Malaysian women.
Approximately 500 women are diagnosed with ovarian cancer every year in our country; of these, 90% are classified as epithelial ovarian cancer.
The remaining 10% consists of germ cell tumours and sex cord stromal tumours, which are less common and generally have a better outlook compared to epithelial ovarian cancer.
Family history is a significant factor as approximately 5-10% of epithelial ovarian cancer cases are due to genetic factors. This means having a close blood relation on either the mother or father’s side of the family who has had breast cancer before the age of 50, or ovarian cancer at any age.
The ovaries, which are two small organs located on both sides of a woman’s uterus, are responsible for releasing eggs every month during a woman’s reproductive years.
They also produce hormones which trigger the secondary sex changes which occur at puberty and maintain reproductive organ function.
When a woman reaches menopause, the ovaries stop releasing the eggs and hormone production decreases.
Epithelial ovarian cancer (hereafter referred to as “ovarian cancer”) in its early stages produces few or non-specific symptoms.
Symptoms and screening
Due to its non-specific symptoms, one of the most significant challenges of ovarian cancer is the absence of a test for early detection which offers a better chance for successful treatment and improved survival rates.
Lack of awareness of symptoms and late stage diagnosis results in many instances of the disease progressing undetected until it reaches an advanced stage – approximately 70% of women are diagnosed at Stage 3 or Stage 4 of the disease, with an overall five-year survival rate of only 30%.
To aid in earlier detection, even vague symptoms should be carefully evaluated. These symptoms include abdominal bloating or fullness, anorexia (poor appetite and loss of weight), nausea, vomiting and urinary symptoms.
However, due to the non-specific nature of these symptoms, most of the women who present themselves with these symptoms would not necessarily be suffering from ovarian cancer.
Unlike the Pap smear which detects pre-cancerous changes in the cervix, or mammograms which detect breast cancer at an early stage, there is no definitive screening test for ovarian cancer.
There is, however, ongoing research evaluating a combination of blood tests for tumour markers together with ultrasound scans with the hope of developing a screening test for the future.
Unfortunately, at the present time, there is not enough scientific evidence to recommend this approach for screening for ovarian cancer.
Screening using the tumour marker CA125 has not been proven to be useful because only 50% of patients with early stages of ovarian cancer have raised levels of CA125. Among patients at an advanced stage of ovarian cancer, 90% of patients have raised CA125 levels, but at such an advanced stage, other signs and symptoms are usually already evident.
Testing for CA125 is also associated with a high false positive rate – i.e. patients may not have cancer, but still exhibit high levels of CA125. In such cases, the patient may needlessly undergo further tests and investigations, which can be costly and invasive.
One percent of healthy women, women in early pregnancy, as well as women with common conditions such as fibroids, endometriosis, kidney disease, lupus, gastrointestinal and liver conditions as well as cancers of the liver, lung, breast and pancreas may have raised levels of CA125.
Hence, this test is not specific enough to detect ovarian cancer and is an ineffective tool.
Diagnosis and treatment
To ensure an accurate diagnosis, a doctor requires the patient’s full medical history to perform a clinical examination, including an abdominal and pelvic examination.
The doctor then arranges other tests such as ultrasound scans, blood tests, including tests for tumour markers, and CT scans. While the number and type of examinations may vary depending on the individual patient, a careful and thorough assessment is essential before embarking on surgery and treatment.
For many patients in the advanced stages of the disease, the tumour often spreads beyond the ovaries to neighbouring organs such as the uterus, bowel and other areas within the abdominal cavity.
Surgery is recommended if cancer is diagnosed; this procedure is called a laparotomy, whereby doctors will remove all or as much of the tumour as possible together with the ovaries, the uterus and omentum (the fat which hangs from the stomach and large intestine).
Removal of the tumour is called “debulking”, and plays an important role in determining the patient’s survival as there is a very close relationship between the amount of tumour left behind after surgery (residual tumour) and the patient’s survival rate.
Simply put, the lesser the amount of residual tumour, the better the chances of survival. In selected patients where the cancer is still in its early stages and confined to only one ovary, it may be possible to perform conservative surgery, which means removing only the cancerous ovary and preserving the uterus and remaining unaffected ovary so that the patient may still have children in the future.
Surgery should be performed by a specialist with the necessary skill, training and experience in treating and managing ovarian cancer. A gynaecologist who specialises in the treatment of women with cancer of the reproductive organs (uterus, ovaries, fallopian tubes, vagina and vulva) is called a gynaecological oncologist.
Several studies have confirmed that better cure rates are obtained when this complex surgery is carried out by a gynaecological oncologist and both the US National Cancer Institute as well as the National Health Service in the United Kingdom have endorsed this recommendation.
Surgery also helps doctors to determine the stage of the cancer; it’s essential for doctors to understand this so they can create an effective treatment plan for the individual patient.
Chemotherapy
Chemotherapy is the use of drugs to stop the growth of cancer cells, either by killing the cancer cells or preventing the cells from dividing, multiplying and spreading.
Patients with very early cancer (stage 1A Grade 1) don’t require chemotherapy. Those with more advanced cancer will benefit from chemotherapy. Most patients will be treated with six courses of chemotherapy. Each course lasts for five to six hours and a course is repeated every three to four weeks.
Some patients, especially those in poor health, may be advised to have neo-adjuvant chemotherapy. This involves giving three courses of chemotherapy first, followed by surgery, and then a further three courses of chemotherapy.
In conventional chemotherapy for ovarian cancer, the drugs are given intravenously. Known as systemic chemotherapy, this treatment decreases the risk of recurrence, prolongs survival and increases the chances of cure.
The most common chemotherapy drugs used for ovarian cancer are carboplatin and paclitaxel, a combination which is well tolerated.
Common side effects of treatment include hair loss (which grows back after the treatment is over), low blood counts and decreased immunity.
Monitoring for side-effects will be carried out at specific intervals by clinical examination and blood tests.
New treatment approach with anti-angiogenesis therapy
Anti-angiogenesis therapy is a form of targeted therapy that has been found to be effective for patients with ovarian cancer.
Angiogenesis or new vessel formation is a pre-requisite for the progression and metastasis (spread) of cancer cells.
A pro-angiogenetic factor in blood, known as vascular endothelial growth factor (VEGF), is related to the progression of the disease and corresponding poor prognosis for ovarian cancer patients.
In 1971, a scientist named Judah Folkman came up with the concept of using drugs called angiogenesis inhibitors to block the growth of tumours by preventing the formation of new blood vessels.
Since then, this form of therapy has been further refined, and subsequent research with anti-VGEF therapy shows that it slows tumour progression, causes resolution of ascites (fluid in the abdominal cavity related to cancer) and makes chemotherapy work better.
In a nutshell
Ovarian cancer is a challenging disease to treat. The cornerstone of treatment is surgery by a trained and experienced surgeon.
Following surgery, most patients will benefit from chemotherapy.
A relatively recent form of targeted therapy, known as anti-angiogenesis inhibitors, has been found to be effective in reducing the progression and metastasis (spread) of cancer cells.
The best hope for successful treatment, however, lies in early detection. At present, ovarian cancer is difficult to detect in its early stages as its symptoms are few and non-specific and there is lack of an effective and proven screening test, hence most patients are only diagnosed at advanced stages of the disease.
Women should be aware of changes in their body and be alert for unusual symptoms. It is said that “ovarian cancer whispers” – some of the signs and symptoms may be mild or subtle.
Evaluation of women with unusual or suspicious signs and symptoms should include assessment by an experienced gynaecologist.
Women should make it a point to have regular check-ups. At these check-ups, unusual symptoms should be discussed and assessed. A pelvic examination should be carried out during routine Pap smears as this may result in the detection of gynaecological problems, including ovarian cancer.
> Dr Suresh Kumarasamy is an obstetrician & gynaecologist/gynaecological oncologist in private practice based in Penang. He is immediate past president of the Obstetrical & Gynaecological Society of Malaysia, a council member of the Asian Society of Gynaecological Oncology and an adjunct associate professor at Penang Medical College.